#triploidy
Text
A ‘twisted’ experience: How KY’s abortion bans are depriving pregnant patients of health care
BY ALEX ACQUISTO
On the way to her 20 week ultrasound, Amy English texted her family group chat inviting guesses on her baby’s biological sex.
“Baby boy English muffin!” her father in-in-law texted.
“I thought boy at first but I’m thinking girl now,” her sister-in-law said. “My official guess is a girl :).”
It was December 28. Earlier that morning, Amy, 31, her husband David, and their 20-month-old daughter Annie had celebrated a belated Christmas at their house in Louisville with family visiting from out of state.
Amy and David had planned this pregnancy, and it was, in a way, perfectly timed. Their baby’s due date was five days after Annie’s birthday. Her children would be two years apart almost exactly to the day — a reality Amy was “ecstatic about.”
Sitting in a fluorescent-lit room inside Baptist Health Louisville, Amy looked for familiar shapes on the screen as an ultrasound tech probed her abdomen. Familiar with radiology in her career as a physical therapist, she has a baseline understanding of how to read ultrasounds: gray shapes usually indicate fluid, and bone shows up as white.
Amy remembers seeing her baby’s arms, legs and the curve of its back. But there was no recognizable outline where the skull should be.
“I couldn’t see the top of my baby’s head,” Amy said in an interview with the Herald-Leader. “I kept waiting for the tech to move the probe in a way where we could see what we should be seeing. I could tell she was searching for it, too.”
Amy had also learned in school about anencephaly, a severe fetal birth defect impacting the brain and skull. A lack of folic acid early in pregnancy increases the likelihood of this happening. This possibility flashed in her mind but she quickly batted it down; she’d been taking her prenatal vitamins, rich in folic acid, for months even before discovering she was pregnant.
The tech paused, then spoke.
“What we’re looking for here is an outline of the baby’s head, and right now I’m not really seeing that,” the woman explained before calling in Amy’s longtime OBGYN.
Over the next few minutes, Amy remembers the room blurring as she heard her doctor use the word “acrania,” which is when a fetus matures through pregnancy without ever developing parts of its skull. It can spur anencephaly, when the brain, too, is underdeveloped and partially missing. Pregnancies with either of these conditions are nonviable.
Amy’s baby, which they learned was a boy, had both. He would not survive into childhood, likely not beyond a few minutes after birth.
This, alone, was devastating news. Her dismay was compounded the next day when she learned that terminating her nonviable pregnancy, even by way of an early induction — a commonplace and provider-recommended method of treatment for such a diagnosis — couldn’t happen.
Even though Amy’s baby would never survive outside her womb, the pregnancy still had a fetal heartbeat — a technicality, considering the diagnosis. Coupled with the lack of immediate threat to her health, her doctors explained they couldn’t induce labor, much less give her an abortion. Kentucky laws forbade it, they said.
“I don’t know what was more shocking: to find out the baby had anencephaly, or that I would have to go out of state to get this care,” Amy said.
Kentucky’s abortion bans do not legally permit the standard of care treatment for a nonviable pregnancy like Amy’s. As a result, doctors must refer patients needing otherwise medically-recommended terminations out of state in droves, along with people desiring elective abortions, according to interviews with seven providers across four hospital systems. Providers who terminate pregnancies in violation of the trigger law can be charged with a felony in Kentucky.
Though this scenario is increasingly common statewide, it’s one arbiters of the state’s laws have yet to remedy, and one lawmakers are not publicly working to resolve.
Kentucky’s trigger law, enacted in late June 2022, criminalizes abortion except to prevent a “substantial risk of death,” or to “prevent the serious, permanent impairment of a life-sustaining organ of a pregnant woman.” The fetal heartbeat law also includes these exceptions but otherwise bans abortion except in a “medical emergency” once fetal cardiac activity begins, usually around six weeks.
Any time a pregnancy is terminated, each law requires a provider to document in writing why it was necessary to, in the case of the six-week ban, “prevent the death of the pregnant woman or to prevent a serious risk of the substantial and irreversible impairment of a major bodily function of the pregnant woman.”
The law permits the Cabinet for Health and Family Services to audit any licensed health care facility to make sure its abortion reporting requirements are “in compliance” with the law.
Both bans allow physicians to use their “reasonable medical judgment” when deciding whether pregnancy terminations are medically necessary. But providers interviewed for this story said that guidance is antithetical with the rest of the law’s limits, which only permit terminations in medical emergencies. There are no exceptions for fetal anomalies, or for the gamut of conditions that may make a pregnancy nonviable but don’t pose an immediate or emergent health risk to a pregnant person.
Moreover, the lack of uniform guidance from the state on what’s considered an emergency means definitions across hospitals sometimes vary, the Herald-Leader found. This has created a legal thicket for health care institutions. As a result, the final say on some critical medical decisions affecting pregnant patients is falling not to medical experts, but to hospital attorneys and administrators, who are worried about legality, liability and reputation.
The Herald-Leader asked the University of Kentucky, UofL Health and Baptist Health for insight into how their respective risk management teams and providers are navigating the laws. None responded to multiple questions about respective protocols for deciding when terminations are legally defensible, or how risk management teams, administrators and providers go about deciding.
“Clinicians have a responsibility to provide compassionate, evidence-based care and counsel to their patients, and also comply with the law,” Baptist said in a statement.
“UofL Health is committed to provide comprehensive health care to all its patients and their families,” UofL said in a statement. “In the case of a nonviable pregnancy that poses a health risk to the mother, we explain options for care while complying with all state and federal laws.”
“Although we cannot discuss when or how our legal counsel gives advice,” UK HealthCare said, “in Kentucky, state law prohibits the University’s physicians and staff from performing abortions except when the mother’s life is in danger. In the case of a nonviable pregnancy, our health care staff work with patients to determine the best course of care for the patient that is consistent with state and federal law.”
‘WE COULD NOT PROVIDE THIS SERVICE HERE’
The morning after Amy learned her baby likely had a fatal birth defect, the diagnosis was confirmed at a second ultrasound with a high-risk specialist. The buoyancy and excitement of the prior day was replaced with dread and grief. Amy remembers the quietness of the room during the second ultrasound, the hollow clicking of the keyboard keys and the intermittent clicking of the computer mouse.
Baptist Health refused to make Amy’s doctor available for an interview. But their conversation was outlined in Amy’s medical records, which were provided to the Herald-Leader.
“I discussed this finding with the patient and offered my sincerest condolences — that this was not compatible with life and that I am so sorry she and her husband are in this situation,” the doctor wrote in her notes. “She was understandably tearful.”
Amy listened as her provider explained her two options: Amy could carry her son to term and deliver him via C-section. He would immediately be taken to palliative care, where he would live a few minutes, maybe hours. Grief counselors would be on standby.
Her second option was to terminate the pregnancy early by way of an abortion or preterm induction. “Choosing not to continue the pregnancy: we discussed that this is also a loving choice for a baby that will certainly not survive,” her doctor wrote.
Pre-trigger law, termination under these circumstances would’ve happened in a hospital, and Amy’s health insurance likely would’ve covered it.
“No part of me wanted to be pregnant anymore,” Amy said. “Every flutter and kick he gave felt like a literal gut punch reminder that I would never get to take him home.”
Strangers were already approaching her at the grocery to ask to touch her stomach. Her patients at work often asked how far along she was. It seemed emotionally unthinkable to continue subjecting herself to a life where, at any moment, she would be forced to repeat that her growing body was nurturing a baby that wouldn’t live, she said.
Termination was what Amy wanted. She erupted into sobs when her doctor told her that under her current circumstances (her life wasn’t immediately threatened, and there was still a fetal heartbeat) it wasn’t an option.
“We discussed that due to our current Kentucky laws, we could not provide this service here,” her doctor wrote in her records.
“I’m sorry, I’m sorry, I’m so sorry,” Amy remembers the specialist saying.
She gave Amy a list of hospitals and clinics in surrounding states that might be able to terminate her pregnancy. Her doctor recommended calling Northwestern Memorial Hospital in Chicago, or another clinic in Illinois, where abortion is widely available.
“Am I just supposed to Google the number, call the front desk and ask, ‘How do I get an abortion at your hospital?’” Amy remembered thinking.
Over the next few days, she, her husband and sister-in-law cold-called a handful of clinics to request a dilation and evacuation abortion, common in the second trimester. But a combination of abortion restrictions in Indiana and Ohio, including gestational limits on when abortion is legal — Amy was 21 weeks along at this point — left her with few options.
Then, Amy’s sister, a nurse anesthetist at Northwestern Medicine Kishwaukee Hospital in Dekalb, west of Chicago, stepped in. Her hospital lacked the equipment for a D&E, but they agreed to induce Amy.
On January 4, after driving close to 400 miles, Amy was induced and gave birth to a son she and her husband named Solomon Matthew. He didn’t cry. His heart beat for about two minutes before it stopped.
‘NOT KNOWING WHAT TO DO’
The Republican-led General Assembly has made no moves to amend or further clarify either abortion ban since both took effect seven months ago, even though the combined impact has harmed patients, doctors have told lawmakers.
The Kentucky Supreme Court still hasn’t issued a preliminary opinion on whether either law infringes on a person’s constitutional right to bodily autonomy and self-determination. Deciding so would temporarily block one or both bans from being enforced. Convened for a regular session through March, the Republican supermajority has yet to file any bills related to reproductive health care access and likely won’t until the high court weighs in.
In the meantime, there’s disagreement about whether or not either ban infringes on providers’ ability to dole out the standard level of care to pregnant patients.
Kentucky Supreme Court Justice Michelle Keller and former Deputy Chief Justice Lisabeth Hughes raised this point during November oral arguments in the pending court case from the state’s two outpatient abortion clinics challenging the constitutionality of both laws.
The trigger law “doesn’t recognize an exception for women who are under the care of a physician who tells them that the standard of care would be to terminate the pregnancy,” Hughes told Solicitor General Matt Kuhn, arguing on behalf of the Attorney General’s office.
As a result, “What’s really happening is physicians in (hospitals) all over the commonwealth are calling the risk managers and attorneys for the hospitals not knowing what to do,” Keller added. “You’re obfuscating what this trigger statute says. There isn’t a strict life of the mother exception.”
The law’s proponents, including Republican Attorney General Daniel Cameron, have cited the provision in the law that allows for use of “reasonable medical judgment” as protecting doctors’ autonomy, and that any challenge to that fact is overblown.
“The law has an explicit health exception, (which) depends on a ‘reasonable medical judgment’ from physicians,” Kuhn told Kentucky Supreme Court Justices that day. There’s been “a lot of misinformation” suggesting the law doesn’t adequately protect a pregnant person’s health, he said, citing two advisories Cameron’s office has issued since both measures took effect. Both clarify that in vitro fertilization, and abortions as treatment of miscarriages, preeclampsia and ectopic pregnancies don’t violate the law.
As for the host of other conditions not mentioned, “we are continuing to work with Kentucky doctors giving guidance on that,” Kuhn said.
But no written evidence of that guidance appears to exist. In response to an open records request from the Herald-Leader, Cameron’s office said this week it had no written or electronic records of communication between the Attorney General’s office and licensed health care facilities or providers regarding the trigger law or six week ban.
‘AN UNNECESSARY PHYSICAL AND PSYCHOLOGICAL RISK’
It was mid June when Leah Martin, 35, discovered she was pregnant with her second child.
Pregnancy at ages 35 and above is considered geriatric. Aware that her age meant she faced a heightened risk, she opted for genetic testing early on to gauge any abnormalities.
Her first ultrasound didn’t raise any alarm. At just over nine weeks, Leah took a prenatal genetic test. The results a week later showed “low fetal fractal numbers,” she said in an interview.
That result, her OBGYN told her, could mean there hadn’t been enough material collected to show a clearer result. It could also signal an abnormality.
Leah, wanting to be judicious, got a more exact genetic test just before 12 weeks. She quickly learned her fetus had triploidy, a rare condition that causes the development of 69 chromosomes per cell instead of the regular 46. It causes not only severe physical deformities, but triploidy stunts development of crucial organs, like the lungs and heart. It means a fetus, if it even survives to birth, will likely not live beyond a few days.
What’s more, Leah was also diagnosed with a partial molar pregnancy, which causes atypical cells to grow in the uterus and, as Leah’s doctors told her, could lead to cancer.
It was mid-July, and Kentucky’s trigger law and six week ban had been in effect for barely two weeks. Leah was familiar enough with what both laws restricted and assumed that because her pregnancy could cause her cancer and was nonviable, she would lawfully qualify as an exception.
So, she weighed her options with her doctors at Baptist Health Lexington, who included Dr. Blake Bradley, her longtime OBGYN.
Similar to Amy’s diagnosis, Leah’s doctors told her that even if she opted to carry the pregnancy to term, her baby “would live a short life in palliative care, most likely never leaving the hospital. It would really be a quite painful existence,” she said.
“I have a 2-year-old at home, and I’m 35, weighing how I would like to expand my family. It seemed like the safest option for me and the compassionate choice for my unborn child was to terminate the pregnancy,” she said.
Like Amy’s, a medically-necessary abortion under these circumstances would typically take place at a hospital, doctors interviewed for this story said. Leah’s health insurance had already agreed to cover it. It was also the quickest way to help Leah to her end goal: getting pregnant again in order to birth a child that would survive.
It was July 21 and Leah was just over 12 weeks pregnant when she learned that Baptist’s legal counsel had blocked her doctors from giving her a dilation and curettage abortion.
“I was told the hospital refused to perform the procedure while the case was being litigated. I was dumbfounded,” Leah said. Hospital lawyers cited an ongoing lawsuit from Kentucky’s two outpatient abortion providers that’s pending before the Kentucky Supreme Court.
According to Leah, hospital providers, relaying the message from administration and risk management, reportedly said if her fetus died on its own, doctors would be able to terminate her pregnancy. But their hands were tied as long as it had a heartbeat.
“People minimize that pregnancy, even under its best circumstances, is associated with life-threatening risks, life-altering risks and emotional impacts,” Bradley told the Herald-Leader. “So, to compel a woman to continue a pregnancy that is by everyone’s assessment, doomed, by definition places that woman at an unreasonable and unnecessary physical and psychological risk, period.”
Baptist Health refused to make Leah’s high-risk doctor available for an interview.
The following Monday, July 25, Leah had an ultrasound at the hospital to confirm what she already knew. As an ultrasound tech probed her abdomen, a wheel of dizzying emotions spun in her head: she desperately wanted a baby, but she didn’t want to birth a child into a painful existence.
Already faced with a gutting dilemma, she felt further burdened by having such an intimate choice ripped from her. And she was furious at now being forced to remain pregnant despite there being no chance for survival, despite the risks continuing such a pregnancy posed to her own body.
She remembers staring at the ultrasound screen waiting to hear the muffled heartbeat of her fetus, racked with guilt because she hoped she wouldn’t.
“It was such a twisted experience being pregnant with a baby I desperately wanted, lying there hoping its heart had stopped,” she said shakily. “It was horrible to have to wish for that in order to receive care. It just felt so unsafe and cruel.”
Leah had already arranged to drive to Chicago to get an abortion when a Jefferson Circuit judge issued a preliminary injunction on July 22, temporarily blocking the state from enforcing both bans. She immediately called EMW Women’s Surgical Center in Louisville — one of the plaintiffs in the lawsuit against the state — and made an appointment.
On Wednesday, July 27, almost 13 weeks pregnant, Leah paid $950 out of pocket for her abortion. Her insurance wouldn’t cover it, since it was considered elective. The following Monday, the Kentucky Court of Appeals overturned the circuit court injunction, reinstating both abortion bans.
After Leah’s abortion, she sent a message to her high-risk doctor. Her doctor responded the following day. Leah shared that correspondence with the Herald-Leader.
“You’ve been on my thoughts a lot,” her doctor wrote. “Words cannot express the dismay I feel right now. I’ve spent my whole adult life learning how to care for mothers in heart wrenching or dangerous situations like yours, and the politics now make it not only impossible, but to work to take care of patients like they deserve — with compassion and science — in these horrible situations is wrong and immoral.”
“I hope your procedure yesterday was smooth, though I know it was hard,” her doctor wrote. “I’m so sorry we could not (were not allowed, rather) to take care of you here.”
#us politics#news#Kentucky Herald-Leader#2023#abortions#Abortion bans#anencephaly#acrania#nonviable pregnancies#kentucky#fetal heartbeat laws#Cabinet for Health and Family Services#dilation and evacuation abortions#Kentucky Supreme Court#Daniel Cameron#triploidy#palliative care#dilation and curettage abortions#Kentucky Court of Appeals#reproductive rights#bodily autonomy
68 notes
·
View notes
Text
April 9, 2024: The Arizona Supreme Court just voted a pre-statehood law from 1864 that will effectively ban all abortion care in the state.
If you need abortion care there is still 45 days to seek abortion care within the state.
arizonaforabortionaccess.org will help refer you to providers that will refer out of state.
My only child was born in Arizona via a late term abortion in 2020 due to Triploidy, a condition that is completely incompatible with life. Having an abortion (vaginal birth with induction) saved my life and my future fertility.
Abortion is healthcare.
3K notes
·
View notes
Note
Anencephaly, major heart defects, major lung defects, trisomy 13, holoprosencephaly, hydranencephaly, renal agenesis, thanatophoric dysplasia, and triploidy. These aren't "disabilities" ; they are death sentences. You are for forcing women who find out a heart breaking truth to know for months they won't be able to have a baby. You are for forcing an infant into the world only to know torture and agony and pain.
You are a monster, full stop. This is not freedom, this is torture.
Allowing a mother to spend every moment she can with her dying child and also giving her the comfort that she did everything she could rather than the guilt of knowing she had her child killed - that’s what you think is torture?
No family should go through this alone, and there are great resources for perinatal hospice that should be made available to parents.
Also, the number of times doctors have been wrong about a diagnosis or survival chance…
Not to mention new options for correcting issues by performing surgery on a baby in utero to save lives:
Heart surgery for Trisomy 13 and 18, surgery for spina bifida, Renal Anhydramnios Fetal Therapy for renal agenesis, placenta-derived stem cell therapy for spinal bifida, just to name a few
My husband’s parents were told he wouldn’t survive. They were told to abort, and they refused. They planned to say goodbye to him in the hospital after he was born. All the family came. He was born, baptized by his grandpa, and rushed to surgery.
As you probably figured out, he survived (since he is now my husband). He has no lingering effects of the condition that doctors said would kill him, except that he only has one kidney (and doctors now say he has normal kidney function because his single kidney grew to compensate).
Doctors aren’t omniscient. Conditions that were death sentences 20 years ago are now treatable. New surgeries and procedures are constantly being developed.
We’re not going to sentence babies to death because a doctor says they’re going to die. Sorry not sorry.
493 notes
·
View notes
Text
I was editing an ask but I accidentally deleted it!
An anon asked if Down’s Syndrome was an intersex variation due to it being a Trisomy, and I would like to correct my original reply.
Down’s Syndrome (Trisomy 21) as a Trisomy wouldn’t be a chromosomal intersex variation because the Trisomy affects chromosome 21 and not 23. I originally mixed up the chromosome name and thought it was intersex- it is not (on it’s own) as far as I’m aware. Trisomy 13 and 18 are also not intersex variations.
However, Triple X Syndrome (Trisomy 23) is an Trisomy intersex condition where the person has 3 X chromosomes.
Triploidy and Tetraploidy are both chromosomal intersex variations but neither are compatible with life.
7 notes
·
View notes
Text
Leah is just... exceptionally brilliant. I don't just say that because I'm her mother, she really is. She understands everything and the underlying emotions and motives and nuance. She knows so much about how the human body works. She's, in a word, precocious.
As you you ALL well know, my pregnancy with her was rough. Medically rough. Medically notable. It's a miracle either one of us is alive let alone both of us.
She knows she was born early. We've shown her pictures of how tiny she was, etc.
The night of her 5th birthday, I am putting her to bed as usual. This night she asks me "why was I born so early? what happened?" and I gave my usual deflection of "honey that's a very complicated story, I'll tell you when you're older" and she looks at me with sincere severity and says, "mama, I'm 5 now."
This broke my heart. How can I tell her even the doctors don't understand what happened? How can I tell her how close to death I was?
So I did my best to make it child friendly. I say, "the pregnancy wasn't going well and I got very sick and they had to get you out of me as soon as possible so they cut you out of my belly."
She seems to accept this and asks why Faye had to be cut out. I told her because I'd already been cut before and it was just safer. She nods.
I've talked a lot about what happened with her but I've never shared the terms because it's so personally identifying if you have access to the right journals. But I was only the 9th woman in all of recorded history to have a pregnancy with a triploid placenta with a normal karyotype fetus. Google triploidy. You'll see.
No one knows how or why it happened. I wasn't meant to live and neither was she. Doctors begged me to abort but I am a stubborn bitch and here we are.
0 notes
Text
Molar Twin Deliveries with Coexisting Fetus at Term: Concerning Two Uncomplicated Cases of Gestational Trophoblastic Tumor, From 2015-2021, In Conakry, Guinea
Abstract
The coexistence of a molar pregnancy with a live fetus is a rare entity of difficult diagnosis and treatment. Continuation of the pregnancy until full-term delivery is possible. We report two cases of twin molar deliveries observed empirically from 2015-2021, in the gynecology-obstetrics department of the Donka national hospital and in the maternity ward of the Jean Paul II hospital in Conakry. The discovery was made on ultrasound of the first trimester of pregnancy and macroscopic examination of the placenta. One of the neonates was alive, a healthy female and the other was polymal formed with facial dysmorphism, omphalocele and sexual ambiguity, fresh stillborn. There was no maternal complication towards a gestational trophoblastic tumor (T.T.G) in both cases. Efforts must be made in the prevention of T.T.G. by screening for twin molar pregnancies with healthy fetuses on transvaginal ultrasound in the first trimester, the dosage of HCG in the face of unexplained metrorrhagia, macroscopic observation of the placenta after each delivery and biopsy sampling of any suspicious placenta.
Introduction
Complete moles with a coexisting fetus, evolving at term with spontaneous vaginal delivery, without fetal and maternal complications, are rare. Early diagnosis of this association leads in the majority of cases to termination of pregnancy on the one hand because of the frequency of triploidy and on the other hand because of the maternal risk and the possibility of progression to persistent trophoblastic disease [1]. We report two particular cases of twin molar deliveries at term without fetal complication and without progression to maternal gestational trophoblastic disease in the gynecology-obstetrics department of the Donka national hospital, the Teaching Hospital (C.H.U) of Conakry and in the maternity ward of the Jean Paul II hospital in Conakry.
Patients and Observations
Case 1
This was Mrs. D.F.B, aged 19, primigravida and primiparous, with no particular history, admitted while in labor at the gynecology- obstetrics department of Donka National Hospital, Conakry Teaching Hospital, with two results of ultrasound performed with a transparietal probe during her pregnancy. These results did not mention any notion of hydatidiform mole or associated congenital malformation. The pregnancy would have progressed normally until its term without maternal or fetal complications. It was only after the delivery of a fresh stillborn, polymalformed (with facial dysmorphism, omphalocele and sexual ambiguity) child, that the macroscopic examination of the placenta made it possible to make the diagnosis of presumptive mole twin by the presence of a normal placenta attached to a vesicular mass characteristic of a mole. The biopsy sample allowed the histological diagnosis of a complete mole. The post molar follow- up had been organized without maternal complication 61 days before the closure of the service for renovation, on October 5, 2015.
Case 2
This was Mrs. H.C, seamstress, 30 years old, gravidity of 5 and parity of 5 including a twin birth and a laparotomy for ruptured ectopic pregnancy (GEU), who came on her own for a consultation for incoercible vomiting, physical asthenia on a menorrhea of 3 three months, June 19, 2020. The clinical examination had objectified a uterine height greater than the age of amenorrhea and dating ultrasound had made it possible to observe, intrauterine, a normal eutrophic fetus of 13 weeks – Amenorrhea (W.A) and a poorly vascularized heterogeneous multicystic mass. The beta HCG serum marker level was 16000IU/l. We had concluded a twin molar pregnancy and animated counseling on the interest of a medical termination of pregnancy to avoid the risks associated with serious maternal complications of trophoblastic tumor including choriocarcinoma. The couple, after a delay of two weeks, had opted to continue the pregnancy until its term. A pregnancy monitoring and childbirth preparation plan had been drawn up with the pregnant woman, whose morphological ultrasound at the 23rd W.A of the second trimester carried out on 03/09/2020, which had objectified a mass of 81 x 97 mm, in previa position. The pregnancy had progressed, without fetal and maternal complications, at 40 WA 2 days and ended with a vaginal delivery of a normal female child, alive and weighing 2830 grams. The woman had benefited from active management of the third stage of labor (TSLM) and digital uterine dissection to confirm the uterine cavity. Macroscopic examination of the adnexa had confirmed the presence of two separate placentas, joined together (Figure 1), one of which appeared normal and linked to the umbilical cord and had a histologically confirmed vesicular mass of “complete mole”. The planned post-molar follow-up was regular with progressive regression of the beta HCG level until negativity on the fortieth day of delivery without any clinical particularity on the closing date of January 31, 2021.
Discussion
The diagnosis of the association of a live fetus with a normal karyotype with a hydatidiform mole is often difficult, especially in the absence of revealing clinical signs [2,3]. The diagnostic modalities of molar twin pregnancy associating a complete mole with a healthy fetus were different due to the early ultrasound detection in the first trimester and the observation of the placenta. The lack of diagnosis of the coexisting mole during pregnancy despite the two ultrasound examinations in the first case would be linked to the age of the ultrasound scanners, which are often second-hand, the technique used (endovaginal in the first trimester or transparietal) and of the operator’s experience in the first observation. Early ultrasound detection made it possible to develop a follow-up plan for pregnancy, childbirth and postpartum in the second case. In the event of a twin pregnancy associating a live fetus and a molar pregnancy, the pregnancy can be continued until term if the patient wishes after having been informed of the risks and the most frequently reported complications (hemorrhages, late miscarriage, fetal death in utero and preeclampsia) [3]. Evacuation of the pregnancy is required only in cases of fetal anomalies or deterioration of the maternal condition [4]. The probability of obtaining a live birth varies between 16 and 56% [5] or 16 and 60% [4] deliveries. The continuation of the pregnancy is against payment given the risks of immediate and distant maternal complications. Close monitoring of the mother and fetus can help achieve a favorable outcome [4]. We accepted monitoring despite the maternal risks for one of our two pregnant women. The two pregnancies resulted spontaneously in the normal delivery at term of a healthy living fetus and another which would have succumbed to its multiple malformations per partum. The most feared complication is progression to gestational trophoblastic disease [1]. The diagnosis of postmolar Gestational Trophoblastic Tumor (G.G.T.) can be made according to criteria such as the persistence of h.C.G detectable more than 6 months after uterine evacuation and the histological diagnosis of choriocarcinoma [5]. According to Ikram Boubess et al., who adopted termination of two of these pregnancies, one remotely progressed to an invasive mole [6]. Regular monitoring of h.C.G levels throughout pregnancy and the postpartum period is necessary to detect GTN [7]. For Suksai M et al., a pregnancy with an initial serum h.C.G level of less than 400,000m.U.I/ml is a good candidate for the continuation of the pregnancy and the achievement of fetal viability [8]. The incidence of post-molar GTN is higher in twin pregnancies combining a complete hydatidiform mole (CHM) and a normal fetus than in single CHM [9].
Conclusion
Spontaneous evolution of the association of molar pregnancy with a live-to-term fetus, without immediate fetal and maternal complications, is possible. The most formidable complication, gestational trophoblastic tumor, choriocarcinoma, was not observed during the study period. The prevention of this complication requires the training of providers in endovaginal ultrasound, its systematic practice in the first trimester of pregnancy, ultrasound and biological monitoring of suspected cases during pregnancy, systematic macroscopic examination of the placenta with biopsy of cases suspect for histological confirmation.
0 notes
Text
Brownsburg family honors daughter through annual toy drive for Riley Hospital
Brownsburg family honors daughter through annual toy drive for Riley Hospital
INDIANAPOLIS — August 28, 2015 is Charlotte Grace Reuzenaar’s birthday.
“I called her sassy pants while she was with us because she was a little fighter, so she had some sass,” Charlotte’s mom, Tiffany Reuzenaar, said.
Charlotte was born with Triploidy syndrome, meaning she had a third complete set of chromosomes. She lived for nine days and was cared for at Riley Hospital for…
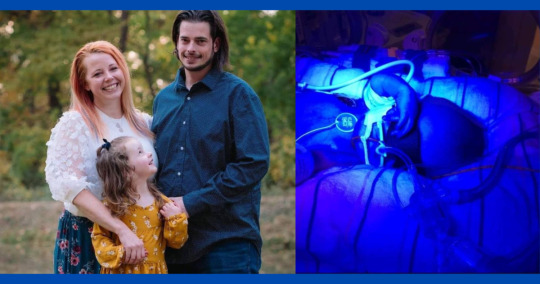
View On WordPress
0 notes
Text
Triploidy (Thể tam bội) là gì? Thai nhi mắc bệnh thường có triệu chứng gì?
Triploidy (Thể tam bội) là gì? Thai nhi mắc bệnh thường có triệu chứng gì? Cùng Siêu thị Kmart tìm hiểu ngay qua bài viết sau nhé. Triploidy (Thể tam bội) là một bệnh lý hiếm gặp ở thai nhi mà các mẹ nên chú ý trong quá trình mang thai. Hôm nay, Siêu thị Kmart sẽ cùng bạn đi tìm hiểu căn bệnh này cũng như các triệu chứng của bệnh nhé. 1 Triploidy (Thể tam bội) là gì? Thể tam bội (Triploidy)...
#sieuthiminikmart
0 notes
Text
Personal Thoughts on Roe v. Wade
I have debated sharing this because what I’m not going to do is get into a debate with any one of you over Facebook. I am a tired mom who loses debates with a five-year-old daily. I have lots of experience trying to reason with people who would happily argue with a brick wall and I’m not doing it here. Not today, Satan.
Many of you know my family. Know my story. Know that building my family was fraught. I don’t think anyone (including me) ever wakes up on a normal day with “ending a pregnancy” tacked to their dream vision board. I certainly didn’t. But eight years ago I found myself living a nightmare. At a routine ultrasound appointment for a child we wanted. Longed for. Prayed for. We found out that our daughter had a terminal condition called triploidy. My trusted OBGYN who had already been with me through multiple losses and my pregnancy with Charlie made her position very clear. My daughter had a zero percent chance of survival. She was suspicious that my pregnancy might be partially molar- a condition that is cancerous. Additionally, as I was already in my second trimester, she was concerned that my inevitable miscarriage would be extremely dangerous should it happen at home. In addition to my doctor, I was also referred to a perinatal specialist who had his own take on my condition. While Margaret’s prognosis remained the same, he told me that whether or not my pregnancy was molar was debatable and couldn’t be determined unless I made the “selfish” decision to proceed with my doctor’s recommendation: a D&C. He made it clear that it was me and me alone who would be morally accountable for whatever came next. Let me be perfectly clear. If Margaret had had any chance at all, I would have risked everything for her. But there I was in a specialist’s office grief stricken over my dying baby, fearing for my own life, and wracked with guilt imposed on me by someone who made it clear that he had a strict personal code of ethics that didn’t really make room to worry about whether I lived or died.
There would never be a scenario where Margaret survived, and in my whole life that is my greatest heartbreak. But there could have been a series of stories that ended with me dying with her had I not had an OBGYN who treated me with compassion and decency. Someone who cared about my life and the lives of my husband and son who could have been left behind.
I survived my greatest tragedy. I can’t help but wonder if I’d be able to say that if it happened today.
0 notes
Text
What types of chromosome abnormalities does PGT-A screen for? | Dr. Manjushri Kothekar | IVF specialist in chembur

To conduct PGT-A, the laboratory most often uses a single nucleotide polymorphism (SNP) microarray and DNA samples from the individuals who contributed the eggs and sperm. Its primary purpose is to ensure that an embryo has the right amount of chromosomes (euploidy). PGT-A looks for full missing chromosomes (monosomy), whole additional chromosomes (trisomy), or a whole extra set of 23 chromosomes in embryos (triploidy). Second, PGT-A looks for missing or additional chromosomes (deletions or duplications). To be detected, these deletions and duplications must be significant, accounting for 15% of the overall length of that chromosome. Finally, PGT-A looks for uniparental disomy (UPD) of chromosomes 6, 7, 11, 14, and 15. When an embryo obtains two copies of a chromosome from one biological parent but no copies from the other, UPD develops. Poor pregnancy outcomes or a child with major health concerns may arise from UPD of these five chromosomes.
Visit- Dr.Manjushri kothekar | IVF specialist in chembur-9769387593
0 notes
Text
I have an interview on Monday with The Copper Courier about Sam and abortion to be released on Triploidy Awareness Day!
We’re going to discuss my abortion and Arizona’s new abortion ban.
11 notes
·
View notes
Text
Help!!
can science side of tumblr please talk to me about unbalanced gametes and why triploids/organisms with an uneven number of chromosome sets are infertile?
I’m glad I’m primarily in human bio/physiology because polyploidy is driving me nuts (and it’s mostly a plant thing)
1 note
·
View note
Text
*deep breath* I think it’s important to be explicitly pro-abortion while still recognizing that eugenics is a thing that exists
non-invasive prenatal testing is often used to diagnose non-terminal conditions like trisomy-21 (down’s syndrome) and spina bifida, and expecting parents are often presented with the option of termination before other resources can be considered, regardless of the birth defects of the specific fetus. That isn’t to say that down’s syndrome and spina bifida can’t be fatal, they definitely can be, and these are specifically high risk pregnancies, but it’s so important for parents to get the full perspective of the health of their child so they can make an informed medical decision about the gestational parent’s health and the fetus’ health. This ties into our medical system too, which has failed disabled people, so parents are faced with choices based on their economic class and access to medical intervention for their children to have the best chances. There are plenty of disabled babies that die due to inaccessibility to treatment like prenatal surgery. We need to be more critical of these arguments in our spaces, because while we should be explicitly pro-abortion, we should also recognize that our system fails disabled fetuses and babies.
Pro-choice arguments in leftist circles often surround the idea of unwanted pregnancy, which is extremely important, but doesn’t establish the full picture that both people who want their pregnancy and those that don’t choose to have abortions/terminations.
we also need to expand our knowledge as leftists of termination for medical reasons and the rights of parents of stillborn children. often enough pro-choice arguments don’t discuss the full extent of (late) termination for medical reasons- they instead focus on the fact that a majority of people that get abortions do so in the first trimester. And while that is an important fact, it’s also important for people to point out that a majority of “late-term abortions” are actually terminations for medical reasons, such as chromosomal conditions like Triploidy (what my child had) and Trisomy 13 & 18, anencephaly, etc, or due to the health condition of the gestational parent.
And I think as leftists we shouldn’t lose sight of that in the fight for reproductive and abortion rights. As a parent of a stillborn child, I’ve seen accounts from gestational parents saying they were forced to carry their terminal and/or dead child because they legally weren’t allowed to induce labor- as it was considered an abortion of the pregnancy, despite the risk of infection, severe pre-eclampsia, hemorrhage, uterine rupture + hysterectomy, and other pregnancy related health problems that come with carrying a terminal or dead baby. It just isn’t right.
#ableism#eugenics#pregnancy#abortion#termination for medical reasons#miscarriage#stillbirth#child death#i just have a lot of thoughts after this experience okay
2K notes
·
View notes
Text
ok
off to genetics & nutrition exam
time to go pray there’s a question about triploid induction/sex manipulation
1 note
·
View note
Text
Warning: this post contains discussion of pregnancy loss and grief.
****************
***********
*******
****
**
I know technically I don't have to update you on what's been happening in my personal life very recently, but I want to, regardless. Mainly because I want to talk about my little boy because I suppose, in a way, the more people that know about him, the more real he feels even though he's no longer here.
On the 4th of January, I gave birth my little boy, Theo. At only 15 weeks, he was born sleeping, weighing only 2oz.
My husband and I made the difficult decision to end the pregnancy after a diagnosis of a rare genetic condition called Triploidy, where instead of the normal 46 chromosomes he had a whole extra set, totalling 69. This meant that it was extremely unlikely Theo would ever survive the pregnancy, but also that the pregnancy itself could be dangerous for me.
It wasn't an easy process. I had complications which led to me needing an emergency procedure in theatre and blood transfusions. But more so than the toll on my physical health, emotionally this has hit my husband and I very hard.
Saying goodbye to him and leaving the hospital was one of the hardest things I've ever had to do, even though I was so eager to get home. I miss him, so much, even though he was with me for such a short time and he was too small to ever really hold.
It's still early days. I know it'll get easier as time goes by, and I'm so grateful for the short time that I had with him.
Thank you to all the people who've taken the time to read this post and all of you who've kept me in your thoughts these past couple of weeks. Thank you most of all to the friends I've made on here who have been such support to me in recent times.
I hope, given time, I'll be able to start posting again here regularly and writing again. Thank you as well for your patience with this, and for still supporting my older works in the meantime.
I hope you're all keeping safe and keeping well with all the god awful stuff going on in the world right now. Be kind to one another 💕💕
128 notes
·
View notes
Text
Hymenoptera - an Order of insects that include wasps, bees, and ants!
I thought it was odd that so many of the eusocial species belong to one Order, especially because there are many wasp and bee species that aren’t eusocial, or even a little social.
But it’s because of their haplodiploidy sex determination! It’s because males have one set of chromosomes and females have two!!
I’ll try to explain
:3 First of all, haploid = one set of chromosomes. Example, a unfertilized human egg cell is haploid. Diploidy = two sets of chromosomes. Examples, a fertilized human zygote; you are an example! (If you are human…) Triploidy exists and can be found in many plants and is irrelevant to this.
In Hymenopterans, sex is determined by how many sets of chromosomes they have! Females have 2 sets. If they reproduce via unfertilized egg, that egg is haploid. Unlike humans, a haploid unfertilized cell developes! Into a male bee! If the female mates with a male, each of their haploid gametes (the egg and sperm) fuse to become diploid. These fertilized eggs become female bees!
THUS, two female daughter bees have very similar DNA! Some from the Queen and some from the male. If this daughter leaves to find her own mate, her children will either have half of her DNA (a haploid son) or half of her DNA and all of her mates DNA (a diploid daughter).
However, a female bee’s sister shares MORE DNA with her than she does her children. Each sister gets half of their DNA from either parent. This results in them sharing various percentages of DNA. They each have 100% of their fathers DNA identically, and 50% of their Queen’s DNA randomly.
Thus, they share at least half of their DNA with their sisters (same % as with their children) BUT can share up to 100% of their DNA, statistically. On average it’s somewhere between 50% and 100%, which is still greater than the percentage they share with their own offspring.
THUS, sisters are more closely related to each other than they are to their daughters! This means that a Hymenoptera is more likely to multiply its genome by raising sisters than it is by raising its own children!!
And thus, the Order contains many species that do this!
I love science!! I love genetics!! I love bees and wasps and ants more than before!! I love learning things and I love biology and I’m gonna go learn more now!!!!!
:3
#ohheyisaidthat#I’m not tagging this with any related terms because I don’t want someone to find my silly ramble 😅😅😅#nevermind! as of feb 2023 i deem this post worthy of being tagged#arthropology
2 notes
·
View notes