#hemolife
Text

Every year on 17 April, World Hemophilia Day is recognized worldwide to increase awareness of hemophilia. Hemophilia doesn't stop us; Let's raise awareness to stop Hemophilia.
#worldhemophiliaday#hemophilia#hemophilialife#hemophiliac#hemophiliamom#hemophiliaday#hemophiliaawareness#whd#hemophiliaproblems#hemophiliacommunity#hemophiliastrong#hemolife#hemofilia#haemophilia#bleedingdisorders#vwd#bloodbrothers#hemophiliarussia#hemophiliab#hemophiliaa#hemophiliawarrior#wfh#tumblrpost
0 notes
Photo

Haemophilia is a rare, but potentially dangerous condition, in which the blood doesn’t clot properly. World Haemophilia Day (April 17) is an International Awareness Day about haemophilia and other bleeding disorders. This year, as the world is fighting the coronavirus, let’s probe further into how haemophilia patients can guard themselves against COVID-19. Am I at an increased risk of catching COVID-19 if I have an inherited blood disorder? No. Your risk is in no way higher than the general population’s. Just like everyone else, practice social distancing, wash your hands and maintain respiratory hygiene to keep yourself safe from COVID-19. Will there be a shortage / non-availability of my medicines due to COVID-19? The medical shops are open. Moreover, the government is doing every bit to ensure that the supply of essentials such as medicines is not getting affected. There’s no need to worry. How important it’s to appraise doctors that I have a bleeding disorder in an emergency? It’s very important considering that COVID-19 patients get isolated. So, be prepared and keep your bleeding disorder card/disease status handy. Does COVID-19 impact the blood clotting mechanism? In the general population, severe cases of COVID-19 that require hospitalization can lead to changes in blood clotting. However, it doesn’t make someone with a blood disorder particularly susceptible. When it comes to COVID-19, you’re not particularly at risk. Stay home and stay safe. If you’re stressed about the situation, talk to a family member or seek the help of a health and wellness counselor. Dr. Sunil Bhat, Director & Clinical Lead – Bone Marrow Transplant, Haemato Oncology, Oncology, Paediatric Oncology, Mazumdar Shaw Medical Center, . #hemophilia #bleedingdisorders #hemophiliac #hemophilialife #haemophilia #hemophiliaawareness #vwd #hemofilia #vonwillebrands #hemophiliacommunity #hemophiliaadvocates #vonwillebranddisease #hemophiliamom #hemolife #hemophiliaa #hemophiliaproblems #hemophiliastrong #hemophiliab #factorix #factorviii #hemophiliawarrior #youthhemophiliahyderabad #worldhemophiliaday #instagram #hemophiliarussia https://www.instagram.com/p/CNv6rZzLVUJ/?igshid=j2qax2qx8rof
#hemophilia#bleedingdisorders#hemophiliac#hemophilialife#haemophilia#hemophiliaawareness#vwd#hemofilia#vonwillebrands#hemophiliacommunity#hemophiliaadvocates#vonwillebranddisease#hemophiliamom#hemolife#hemophiliaa#hemophiliaproblems#hemophiliastrong#hemophiliab#factorix#factorviii#hemophiliawarrior#youthhemophiliahyderabad#worldhemophiliaday#instagram#hemophiliarussia
0 notes
Photo
Over the weekend getting it in on Xbox. . . . 2 squad wins with @whatashark and the boys. Will start streaming @pubg @xbox on @twitch hopefully this weekend! . . . #dozerdh #thehemogamer #hemolife #hopeforhemophilia #factorup #hemophilia #hemophiliac #hemoawareness #hemo #hemophiliaawareness #bleeder #bleedingdisorders #bleedingdisorder #gaming #gamer #youtubegamer #youtube #livestreamer
#hemolife#gamer#hemophiliaawareness#hopeforhemophilia#bleedingdisorders#youtube#hemophiliac#bleedingdisorder#thehemogamer#hemoawareness#youtubegamer#livestreamer#dozerdh#gaming#hemo#hemophilia#bleeder#factorup
1 note
·
View note
Photo

Free Ebook. Go to www.wineracupuncture.com to download. We go above and beyond for our patients. Enjoy and please share. Life doesn’t have to be a pain and you do t need to be stressed. Let Winer Acupuncture help. #amazon #motivated #instafit #love #author #infusions #bleedingdisorder #booknerd #hemolife #flexibledieting #bookworm #weightloss #books #authorsofinstagram #bookshelf #ebook #entrepreneur #booklover #book #bibliophile #acupuncture #bookstagram #stress #stressrelief #bookish #reading #fitness #writer #kindle #writersofinstagram 👌👌👌👍👍👍👍 https://www.instagram.com/p/Bwj9pHIH9EQ/?utm_source=ig_tumblr_share&igshid=1wclcuge5f6do
#amazon#motivated#instafit#love#author#infusions#bleedingdisorder#booknerd#hemolife#flexibledieting#bookworm#weightloss#books#authorsofinstagram#bookshelf#ebook#entrepreneur#booklover#book#bibliophile#acupuncture#bookstagram#stress#stressrelief#bookish#reading#fitness#writer#kindle#writersofinstagram
0 notes
Photo
It’s No Mans Wednesday!!! #dozerdh #thehemogamer #hemolife #hopeforhemophilia #factorup #hemophilia #hemophiliac #hemoawareness #hemo #hemophiliaawareness #bleeder #bleedingdisorders #bleedingdisorder #gaming #gamer #youtubegamer #youtube #livestreamer
#hemo#factorup#youtubegamer#hemophilia#hemophiliac#livestreamer#hemolife#dozerdh#bleeder#bleedingdisorders#bleedingdisorder#youtube#hemophiliaawareness#gaming#gamer#thehemogamer#hemoawareness#hopeforhemophilia
0 notes
Photo

#Repost @bmxthegardennj with @repostapp ・・・ #gardengrownnj #hoodie #new #represent #sponsored #naturallyproud #gardenstate #njallday #973 #mcraemanagement #hashtagwhores #hemolife #oss #thecomeup #camo #walking #billboards #everyonesfuckin #movment #bmx #bikelife #bmxnewjersey #merritt #ilovebmx #Jerseyshore #2017 #mmllc #RIDEBMX
#hashtagwhores#ilovebmx#973#movment#camo#hemolife#thecomeup#oss#everyonesfuckin#new#sponsored#represent#billboards#bmxnewjersey#merritt#jerseyshore#hoodie#mcraemanagement#njallday#bikelife#bmx#repost#gardengrownnj#ridebmx#walking#2017#mmllc#naturallyproud#gardenstate
0 notes
Photo
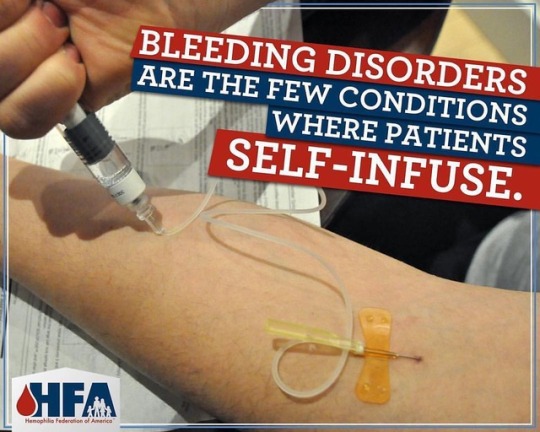
Took me 21 years to be able to self infuse. I was always scared I would shoot air into my veins and die. Basically the meaning of this post is to spread awareness to the community about bleeding disorders; which I was born with and the reason to why I medicate with cannabis. #hemolife #hemophiliasucks #hemophiliafederationofamerica #gasonlyinc #medicalmarijuana #mmj #chronicpain #cannabiscures #cannabisheals
#hemolife#chronicpain#hemophiliafederationofamerica#gasonlyinc#hemophiliasucks#mmj#medicalmarijuana#cannabiscures#cannabisheals
0 notes
Photo
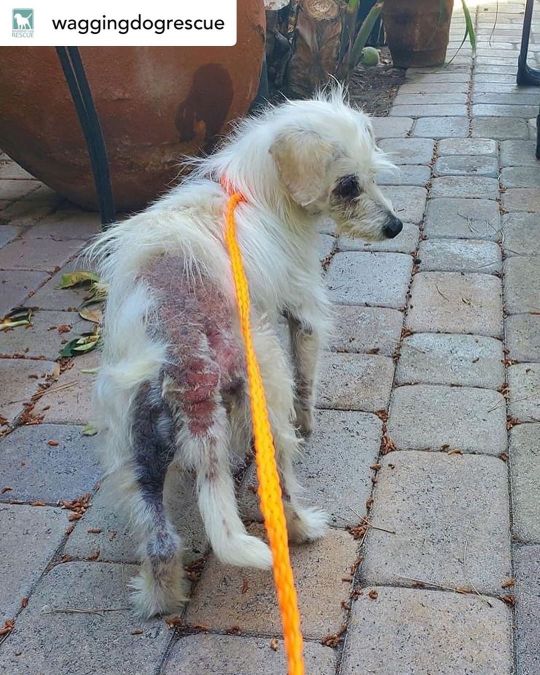
Posted @withregram • @waggingdogrescue Amidst all the DiscoverMe Project™ stuff we’ve been doing nonstop since mid-March, we’re still saving lives through our regular rescue program thanks to fosters saying, '𝘠𝘌𝘚, 𝘐’𝘭𝘭 𝘤𝘢𝘳𝘦 𝘧𝘰𝘳 𝘵𝘩𝘪𝘴 𝘣𝘢𝘣𝘦 𝘶𝘯𝘵𝘪𝘭 𝘴𝘩𝘦’𝘴 𝘩𝘦𝘢𝘭𝘵𝘩𝘺 𝘢𝘨𝘢𝘪𝘯 𝘢𝘯𝘥 𝘧𝘪𝘯𝘥𝘴 𝘵𝘩𝘦 𝘱𝘦𝘳𝘧𝘦𝘤𝘵 𝘧𝘢𝘮𝘪𝘭𝘺!’ So, we’d like to introduce you to our newest Wagging Dog. Please welcome sweet 𝗭𝗜𝗡𝗡𝗜𝗔 to our fam! 💖🐶🌸 This pretty 8 lb senior is being seen by our new OC vet today. We’re super excited to have one of our dogs at Hemopet Holistic Care in Garden Grove. We love the incredible pioneer Dr. Jean Dodds' Hemopet, Petlifeline, Hemolife & Nutriscan, and she has a team of amazing integrative vets so Zinnia’s in the best hands! Our poor girl arrived at OC Animal Care a week ago, suffering from long neglect, extremely thin. We originally thought she was going to be a DiscoverMe Dog™ but as soon as her DMP foster laid eyes on her, she offered to care for this pup until we return her to good health and find an awesome family to cherish her. YAY Zinnia! Like our GSD Blume, we chose a flower themed name for our new girl in anticipation of her blossoming this spring. 🌷 Zinnia is deaf. Our vet thinks she’s around 12 yrs old, a bit more than 7 estimated at the shelter. She has some age related eye changes but no cataracts. A mid-grade heart murmur, yucky grill, extremely overgrown nails curling back on themselves, and of course that skin. Good grief :’( Zinnia is so uncomfortable, so itchy. We’re anxious for her to feel better and to see her beautiful white fur filling in. 🙏 The estimate for today’s exam and preliminary diagnostics is $850-900 and we’d be so grateful for your help providing this critical care for sweet Z. We’ll be anxiously awaiting lab results (hopefully tomorrow) so we have an idea of what her lil body is dealing with and how we can best provide for her return to total wellbeing. We know she has a dental and spay in her future, as long as her ticker checks out. Add in a heart ultrasound too. 💰 #TaxDeductible #donations can be made via this fb post or - PayPal - [email protected] venmo https://www.instagram.com/p/B_5o4aNg-Y4/?igshid=1h64514homrjo
0 notes
Text
Myasthenia Gravis in Dogs

Myasthenia Gravis is a deficiency of the neurotransmitter, acetylcholine, that results in a neuromuscular junction dysfunction. Think of it like talking to toddlers: they do not have enough words to communicate effectively. In this instance, there is not enough acetylcholine sending vital information from the nerves to the muscles. This results in muscle weakness of the limbs, face, and/or the esophagus.
Symptoms
The symptoms – which are progressive – can vary from dog to dog.
Megaesophagus – relaxing of the esophageal muscle so that food cannot be pushed by normal muscle contraction down into the stomach. Dogs can develop aspiration pneumonia from inhaling regurgitated food.
Pharynx laxity – changes occur to the bark
Limb muscle weakness and stiffness – use of the muscles exhaust the limited amount of acetylcholine available. Affected dogs will usually exhibit shortened strides and stiffening limbs during exercise, but also muscle weakness after exercise. As the disease progresses, the periods of exercise exertion shorten while rest time lengthens. This can lead to paralysis.
Facial weakness – inability to blink; drooping lip; and facial paralysis
Drooping tail
Trouble controlling urine stream or squatting
Lethargy
Forms of Myasthenia Gravis
Two forms of Myasthenia Gravis have been identified: congenital (hereditary) and acquired.
Congenital Myasthenia Gravis
Congenital Myasthenia Gravis requires that both parents carry an autosomal recessive trait that creates a deficit in the number of the acetylcholine receptors. It is a very unfortunate condition:
Genetic testing does not exist yet to screen out the recessive trait
Diagnosis is best done with muscle biopsy of the afflicted
The onset of generalized muscle weakness starts around 6 – 8 weeks of age
It is progressive
Treatment is available but usually pups do not respond
Death often occurs before puberty
Jack Russell Terriers, Springer Spaniels, Smooth Fox Terriers and Dachshunds have all been identified as carriers of the gene. Interestingly, it has been noted that sometimes Dachshunds can spontaneously recover. Spontaneous recovery or not, these dogs should not be bred and the parents should never be used for breeding with any dog.
Acquired Myasthenia Gravis
Acquired Myasthenia Gravis is an immune-mediated (autoimmune) neuropathy (disease of the nerves). The body produces autoantibodies that attack and destroy the acetylcholine receptors specifically. Like most immune-mediated diseases, we do not know what outside forces (food, infections, chemicals, vaccines, environment, etc.) trigger the body to produce these antibodies that attack itself, but believe there is also a genetic component. In the instance of Myasthenia Gravis, it might be an abnormal thymus gland but researchers are not certain yet.
A dog’s thymus gland functions similarly to that in humans. It is a vital organ in the development of the immune system since it builds up the T-lymphocytes (T-cells) to help fight infection and other immune challenges. Once this developmental process is complete, the thymus stops active production and stays dormant. In humans and dogs with myasthenia gravis, it has been observed that the thymus gland remains large and is abnormal (forms a thymoma).
Researchers believe the thymus gland may give incorrect instructions to developing immune cells, ultimately resulting in autoimmunity and the production of the acetylcholine receptor antibodies, thereby setting the stage for the attack on neuromuscular transmission.
We can also assume that there is a genetic predisposition because we find it more often in Golden Retrievers, Labrador Retrievers, Akitas, Miniature Dachshunds, Scottish Terriers, German Shorthaired Pointers, Shetland Sheepdogs, and Collies. However, it must be remembered that any dog of any breed can develop Myasthenia Gravis.
For some reason, we often see peaks of Acquired Myasthenia Gravis, between the ages of 2 – 4 and then again from 9 – 13 years of age. Unfortunately, pet parents may think it is just the signs of aging of their senior dog, and not seek out proper diagnosis, management and treatment.
With this form of Myasthenia Gravis, we break it down further into three groups:
Mild or Focal – only one body part is afflicted and it is usually the esophagus
Moderate Generalized – limb weakness with or without megaesophagus
Severe Generalized or Acute Fulminating – rapidly progressive and usually fatal
Diagnosis
As stated previously, the best way to diagnose Congenital Myasthenia Gravis is with a muscle biopsy that is sent to Dr. Diane Shelton at the University of California San Diego’s Comparative Neuromuscular Laboratory.
Fortunately, a blood test exists for the Acquired form. This blood test, AChR, checks for the autoantibodies that are destroying the acetylcholine receptors. Remember, the congenital form does not have the autoantibodies. The AChR specificity rate is 98%. If the veterinarian is fairly certain that your dog lands within this 2% zone, other tests are available such as the Tensilon Response Test to see if the muscles move after administering edrophonium chloride, and electrodiagnostic testing to see if electrodes stimulate the muscles to respond at various levels. He can also retest with the AChR test a couple of weeks later.
Before performing these secondary or follow-up tests, I would also consider thyroid disease as a possible cause of these symptoms. Thyroid dysfunction can cause neuropathies such as megaesophagus and muscle weakness. Indeed, hypothyroidism could be concurrent with Myasthenia Gravis. Thus far, we believe they are separate conditions and that one does not precipitate the other. Regardless, I recommend a complete thyroid panel that measures the hormones T4, FT4, T3 and FT3, and the thyroid autoantibody, TGAA, at either Hemopet’s Hemolife Diagnostic Laboratory, Michigan State University, or another veterinary reference diagnostic laboratory.
Treatment
Treatment outcomes for Myasthenia Gravis are variable. Fortunately, while many dogs have spontaneous remissions, the stated 87% rate of spontaneous remissions within the first four months is of concern. It could relate to a number of reasons such as incorrect original diagnosis, another cause (e.g. tick-borne paralysis, vaccines), and giving optimal treatment dosage and supportive care by the pet caregiver. Secondly, the diagnostic group involved – focal, moderate, or severe – also impacts the outcome.
Once diagnosis is confirmed, veterinarians can prescribe anticholinesterase agents. Basically, the body has a naturally occurring acetylcholinesterase enzyme that breaks down acetylcholine, which is needed to put the brakes on the neurotransmission. Think about it, if acetylcholinesterase did not exist, we would have muscle spasms or facial tics all the time. So, if we stop or slow the production of it, the acetylcholine has time to replenish and do its job.
Use of other drugs such as glucocorticoids (a class of corticosteroids) and other immunosuppressive drugs is controversial and inadvisable. They can enhance certain symptoms like muscle weakness or cause side effects like weight gain, instead of effectively treating the condition.
The most innovative procedure to date is therapeutic plasma exchange (TPE). Basically, the plasma containing the autoantibodies is removed and exchanged with fresh healthy canine donor plasma. However, it is not a cure for Myasthenia Gravis, expensive and usually requires going to a research veterinary institution.
Other supportive care really comes down to a daily ritual depending upon what part of the body is affected. For instance, megaesophagus requires fine-tuned care that includes slow eating, swallowing small chunks of food whole, lifting the food and water bowls to chest height, and possibly using a Bailey Chair to sit the dog in an upright position.
Myasthenia Gravis demands patience and commitment from the pet caregiver. Remember, it is a progressive condition that does not have a cure but we can try to slow the progression and side effects with the right supportive care and medications for a longer, quality life.
W. Jean Dodds, DVM
Hemopet / NutriScan
11561 Salinaz Avenue
Garden Grove, CA 92843
References
Kumar, Rajesh et al. “Therapeutic Plasma Exchange in the Treatment of Myasthenia Gravis.” Indian Journal of Critical Care Medicine: Peer-reviewed, Official Publication of Indian Society of Critical Care Medicine 19.1 (2015): 9–13. PMC. Web. 15 Jan. 2017. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4296418/.
"Myasthenia Gravis." National Institutes of Health. U.S. Department of Health and Human Services, n.d. Web. 15 Jan. 2017. http://www.ninds.nih.gov/disorders/myasthenia_gravis/detail_myasthenia_gravis.htm.
"Myasthenia Gravis." VetMed. University of California Davis, n.d. Web. 15 Jan. 2017. http://www.vetmed.ucdavis.edu/vsr/Neurology/Disorders/Myasthenia%20Gravis.html#Pubs.
Purves D, Augustine GJ, Fitzpatrick D, et al., editors. Neuroscience. 2nd edition. Sunderland (MA: Sinauer Associates; 2001. Acetylcholine. https://www.ncbi.nlm.nih.gov/books/NBK11143/.
4 notes
·
View notes
Photo
First @thehemogamer stream is in the books!. . . Now I’ll admit I was quite rusty but had a ton of fun. Thanks to all who came and checked it out. Doing it all over again tonight!. . . #Repost @thehemogamer (@get_repost) ・・・ First stream went okay...If you like rust buckets. Got some kills tho! . . I want to thank everyone who joined me last night, it was a lot of fun for my first stream and we covered quite a few Hemo topics. . . . #dozerdh #thehemogamer #hemolife #hopeforhemophilia #factorup #dozerdiehappy #hemogamer #hemophilia #hemophiliac #hemoawareness #hemo #hemophiliaawareness #bleeder #bleedingdisorders #bleedingdisorder #factor8 #bloodbrothers #bloodbrother #hemofamily #bloodsister #bloodsisters #vmd #vonwillebrands #vonwillebrandsdisease #factor #gaming #gamer #youtubegamer #youtube #livestreamer
#hemo#youtube#hemolife#bleedingdisorders#thehemogamer#hemogamer#bloodsisters#hemofamily#dozerdiehappy#hemophiliac#gaming#vonwillebrands#bloodbrother#bloodsister#hemophilia#youtubegamer#livestreamer#dozerdh#hemoawareness#hopeforhemophilia#vonwillebrandsdisease#bleeder#bloodbrothers#bleedingdisorder#factor#repost#hemophiliaawareness#factor8#factorup#vmd
1 note
·
View note
Photo

When you bang up your shoulder getting into your car, and it happens to be prophy day.... . . . Stream starts in 30! Find out what I’m playing...link in the bio #dozerdh #thehemogamer #hemolife #hopeforhemophilia #factorup #hemophilia #hemophiliac #hemoawareness #hemo #hemophiliaawareness #bleeder #bleedingdisorders #bleedingdisorder #gaming #gamer #youtubegamer #youtube #livestreamer
#hemoawareness#hemophiliac#hemophilia#hemo#factorup#hemolife#hopeforhemophilia#dozerdh#gaming#livestreamer#bleedingdisorders#thehemogamer#hemophiliaawareness#youtubegamer#gamer#youtube#bleeder#bleedingdisorder
0 notes
Photo

Handed out some salt during my test stream. #fortnite #fortnitebattleroyale . . . I will be doing some Live Test Streams next week of Battlefront 2 and Fortnite. Be sure to follow me on Twitter I find out what time as the streams will not be scheduled! . . . These test streams will be the foundation for The Hemo Gamer. This project started a few short months ago and it’s been everything to me. I haven’t felt this way since plying in a band and it’s amazing. Please check out the link in my bio and help support this mission. 2018 will begin scheduled live streams and some HUGE announcements. Stay tuned..... . #thehemogamer #dozerdh #hemophilia #bleeder #hemophiliaawareness #factorup #hemolife #hopeforhemophilia #gamer #gaming #ps4 #livestream #youtubegaming #youtubegamer #youtubegamers #battlefront2 #starwars #documentdontcreate
#gamer#hemophilia#hemophiliaawareness#bleeder#hopeforhemophilia#fortnite#hemolife#ps4#fortnitebattleroyale#livestream#youtubegaming#youtubegamers#battlefront2#factorup#gaming#documentdontcreate#starwars#youtubegamer#dozerdh#thehemogamer
0 notes
Video
So I’ve been a little M.I.A. For a while...sorry bout that, keeper hitting snooze. SO HERES SOME NEWS! . . . The Unite for Bleeding Disorders wall is happening in Chicago on September 15th. Be sure and get the link in my description to snag our teams T-shirt from amazon! . . . Also....streaming schedule will be worked on this week so expect some streams beginning in September!!! . . #dozerdh #thehemogamer #hemolife #hopeforhemophilia #factorup #hemophilia #hemophiliac #hemoawareness #hemo #hemophiliaawareness #bleeder #bleedingdisorders #bleedingdisorder #factor8 #bloodbrothers #bloodbrother #hemofamily #bloodsister #bloodsisters #vmd #vonwillebrands #vonwillebrandsdisease #factor #gaming #gamer #twitch #youtube #livestreamer #livestream https://www.instagram.com/p/Bm_3F9xgUWE/?utm_source=ig_tumblr_share&igshid=1r30u3vrw42w8
#dozerdh#thehemogamer#hemolife#hopeforhemophilia#factorup#hemophilia#hemophiliac#hemoawareness#hemo#hemophiliaawareness#bleeder#bleedingdisorders#bleedingdisorder#factor8#bloodbrothers#bloodbrother#hemofamily#bloodsister#bloodsisters#vmd#vonwillebrands#vonwillebrandsdisease#factor#gaming#gamer#twitch#youtube#livestreamer#livestream
0 notes
Photo

First full week of streaming is in the books. . . #dozerdh #thehemogamer #hemolife #hopeforhemophilia #factorup #hemophilia #hemophiliac #hemoawareness #hemo #hemophiliaawareness #bleeder #bleedingdisorders #bleedingdisorder #gaming #gamer #youtubegamer #youtube #livestreamer
#hemoawareness#bleedingdisorder#hemophiliaawareness#bleeder#thehemogamer#livestreamer#hemo#hopeforhemophilia#hemophiliac#hemolife#factorup#gaming#youtube#dozerdh#gamer#bleedingdisorders#youtubegamer#hemophilia
0 notes
Photo

No Mans Sky day 2 !?!?! . . . #dozerdh #thehemogamer #hemolife #hopeforhemophilia #factorup #hemophilia #hemophiliac #hemoawareness #hemo #hemophiliaawareness #bleeder #bleedingdisorders #bleedingdisorder #gaming #gamer #youtubegamer #youtube #livestreamer
#thehemogamer#hemophilia#hemolife#youtubegamer#bleedingdisorder#hemo#bleeder#youtube#hemophiliac#dozerdh#factorup#hemophiliaawareness#gaming#gamer#bleedingdisorders#hopeforhemophilia#hemoawareness#livestreamer
0 notes
Photo
It’s No Mans Wednesday!!! #dozerdh #thehemogamer #hemolife #hopeforhemophilia #factorup #hemophilia #hemophiliac #hemoawareness #hemo #hemophiliaawareness #bleeder #bleedingdisorders #bleedingdisorder #gaming #gamer #youtubegamer #youtube #livestreamer
#hopeforhemophilia#hemophiliac#hemo#bleedingdisorders#bleedingdisorder#gaming#dozerdh#hemophiliaawareness#factorup#thehemogamer#livestreamer#hemolife#hemoawareness#youtube#hemophilia#gamer#youtubegamer#bleeder
0 notes